What is a Herniated Disc?
Your spine is made up of a series of bones called vertebrae, stacked on top of one another and separated by soft, cushion-like structures known as intervertebral discs. These discs serve as the spine’s shock absorbers, protecting the vertebrae during everyday movement such as bending, twisting, and lifting, while keeping the spine flexible and properly aligned.
A herniated disc (also referred to as a slipped disc, ruptured disc, or prolapsed disc) occurs when the soft inner material of the disc pushes through a crack or weak spot in the outer layer. When this happens, the displaced disc material can press against nearby spinal nerves, triggering a range of painful and sometimes debilitating symptoms.
Herniated discs can occur anywhere along the spine, but they are most common in the lower back (lumbar spine) and the neck (cervical spine). If you are experiencing neck or back pain, numbness, or weakness in the arms or legs, Shore Spine & Pain serves Lakewood, NJ and Shrewsbury, NJ with the diagnostic expertise and minimally invasive treatment options to identify what is causing your symptoms and address it directly.
What Causes a Herniated Disc?

Herniated discs can result from a variety of factors, ranging from the gradual wear of aging to sudden traumatic injury. Understanding the underlying cause is an important step in developing an effective treatment plan.
- Age-Related Degeneration: The most common cause of a herniated disc is the natural aging process. As we get older, intervertebral discs gradually lose their water content, becoming stiffer, thinner, and less flexible. This process, called disc degeneration, makes the outer layer of the disc more susceptible to cracking or tearing, even under normal stress.
- Physical Strain and Improper Lifting: Lifting heavy objects using your back rather than your legs places enormous stress on the lumbar discs and can cause an acute herniation. Twisting or turning while lifting amplifies this risk significantly. Even everyday activities like bending awkwardly, reaching overhead, or pulling heavy items can be enough to cause a disc to rupture if the outer layer is already weakened.
- Repetitive Motions and Occupational Hazards: Those who perform repetitive physical tasks at work face a heightened risk of disc herniation due to the cumulative stress placed on the spine over time. Prolonged sitting, particularly with poor posture, can also increase pressure within the lumbar discs, gradually weakening the disc structure.
- Traumatic Injury: A sudden, forceful impact such as a car accident, a hard fall, or a sports collision can cause an immediate disc herniation. Trauma can rupture even a healthy, well-hydrated disc, though pre-existing degeneration increases the likelihood of injury from a traumatic event.
- Lifestyle and Genetic Factors: Excess body weight places added stress on the lumbar spine and accelerates disc degeneration. Smoking is also associated with decreased disc health, as it reduces blood supply and nutrient delivery to spinal tissues. Additionally, genetics play a role, as some individuals are predisposed to disc problems due to the inherited structure and composition of their spinal tissues.
Symptoms of a Herniated Disc
Herniated disc symptoms vary considerably depending on where in the spine the herniation has occurred, how large it is, and whether it is pressing on a nerve.
- Lower Back (Lumbar) Herniation: A herniated disc in the lumbar spine is the most common type and frequently causes sciatica, a sharp, burning, or shooting pain that radiates from the lower back through the buttock and down one leg, sometimes reaching the foot. Tingling or numbness along the path of the affected nerve is also common, as is muscle weakness in the leg or foot that can affect walking, standing, or climbing stairs. Symptoms are often worsened by sitting, bending forward, sneezing, coughing, or straining, and may improve with movement or lying down.
- Neck (Cervical) Herniation: When a disc herniates in the cervical spine, symptoms often radiate into the shoulder, arm, and hand on the affected side. A deep ache in the neck and shoulder is typical, along with burning, tingling, or numbness traveling down the arm into the fingers. Gripping objects may become difficult due to muscle weakness. Headaches originating at the base of the skull are also reported in some cases.
- General and Localized Symptoms: Beyond nerve-related symptoms, a herniated disc can cause localized pain and stiffness at the site of the herniation. Range of motion is often limited, and certain positions or movements can provoke sharp flares of pain. Muscle spasms near the affected area are also common.
- Cauda Equina Syndrome: In rare but serious cases, a large herniation can compress the bundle of nerves at the base of the spinal cord. Symptoms include loss of bowel or bladder control, severe or rapidly worsening weakness in both legs, and numbness in the groin or inner thighs. This is a medical emergency requiring immediate attention.
Treatments We Offer for Herniated Disc

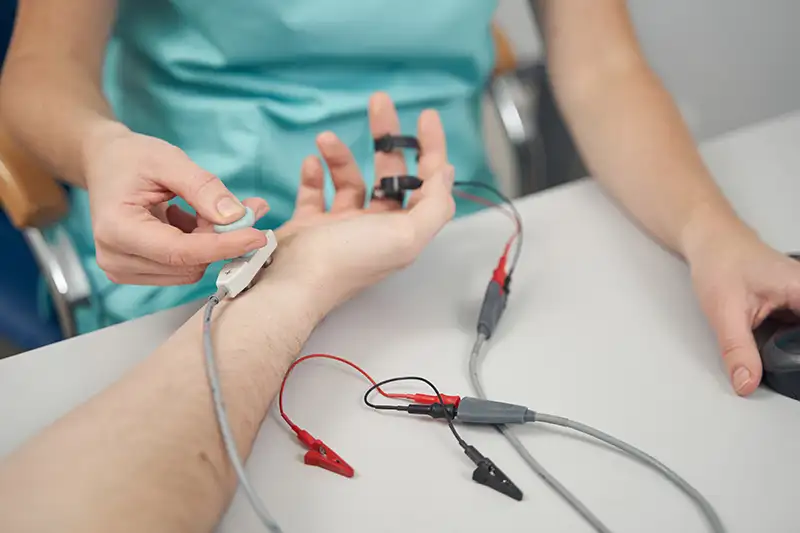
The vast majority of herniated disc cases improve significantly with time and appropriate non-surgical care. At Shore Spine & Pain in Lakewood, NJ and Shrewsbury, NJ, Dr. Woska evaluates the location and severity of the herniation, the nature and duration of symptoms, and overall health before recommending a course of action. When needed, Discography and Electrodiagnostic Testing (EMG) help confirm the disc as the source of pain and assess the extent of nerve involvement before treatment begins.
Interventional Pain Management:
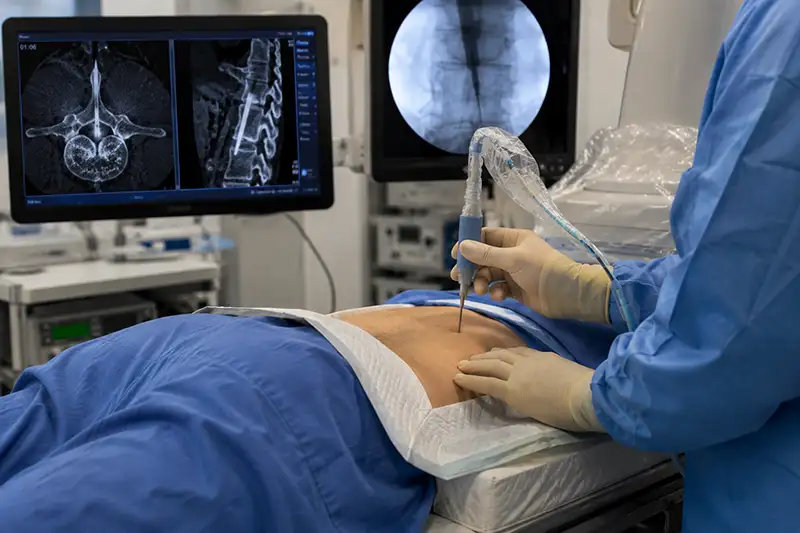
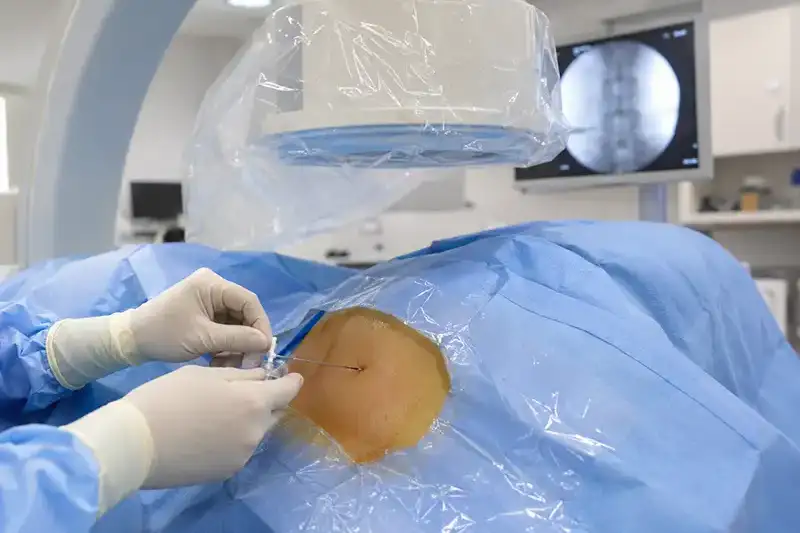
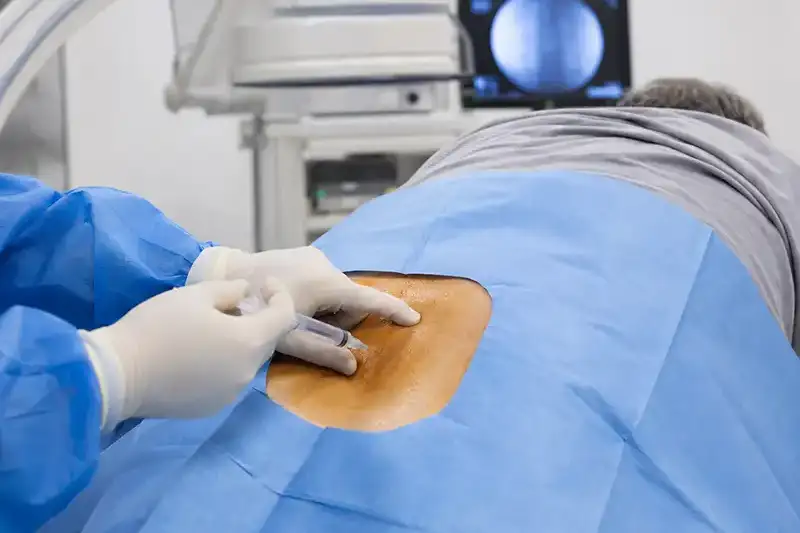
- Epidural Steroid Injections: When conservative measures do not provide adequate relief, an epidural steroid injection can be a highly effective next step. A corticosteroid is delivered directly into the epidural space surrounding the compressed nerve, reducing inflammation and providing targeted relief. This can significantly reduce radicular symptoms such as sciatica, with relief lasting several weeks to several months.
- Facet Joint Injections: When localized spinal pain accompanies a herniated disc, a facet joint injection can help identify and address pain originating from the joints adjacent to the affected disc, providing both diagnostic clarity and symptomatic relief.
- Radiofrequency Ablation: For cases where facet joint involvement is confirmed, radiofrequency ablation uses targeted heat energy to interrupt pain signals from the affected nerves, offering longer-lasting relief than injection alone.
Surgical Options:
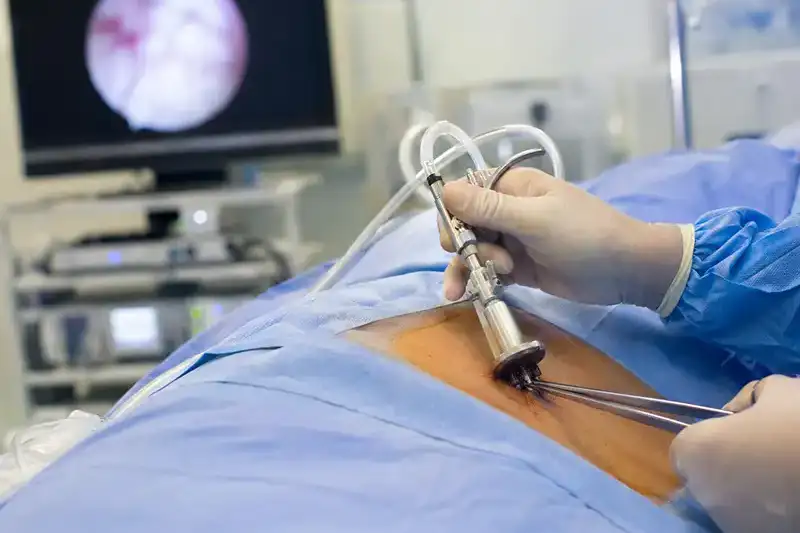
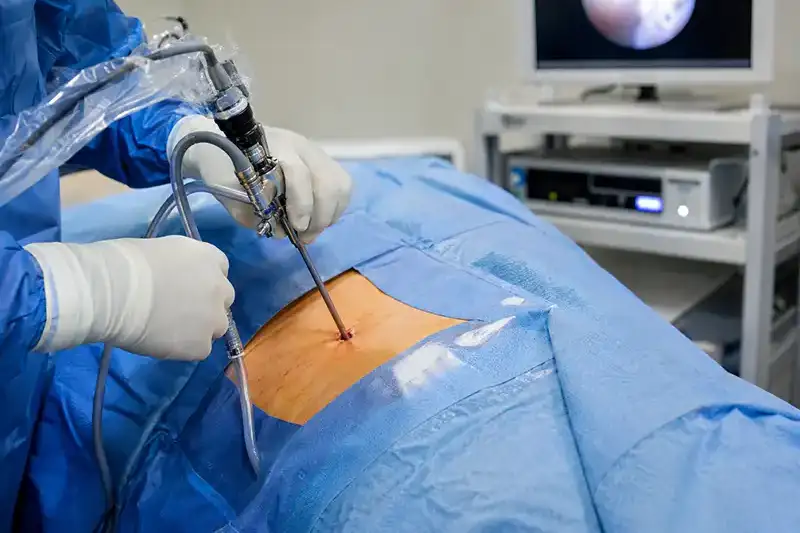
- Discectomy: For those who do not respond adequately to conservative and interventional treatments, or whose symptoms are severe, rapidly worsening, or associated with significant neurological deficits, a minimally invasive discectomy may be recommended. The portion of the herniated disc pressing on the nerve root is carefully removed through a small incision using a microscope or endoscope, minimizing disruption to surrounding tissues. Most cases see rapid relief of radiating arm or leg symptoms following the procedure.
- Spinal Cord Stimulation: For those with persistent or refractory pain following other treatments, spinal cord stimulation offers a long-term option for managing chronic disc-related nerve pain.
- Peripheral Nerve Stimulation: In select cases where nerve pain remains difficult to control, peripheral nerve stimulation can provide targeted relief by modulating pain signals along the affected nerve pathway.
No matter where you are in your herniated disc journey, Shore Spine & Pain is committed to providing compassionate, expert care aimed at restoring your quality of life. Your treatment plan will be crafted specifically for you, with your goals, your timeline, and your wellbeing at the center of every decision.
Frequently Asked Questions about Herniated Discs
What is the difference between a herniated disc and a bulging disc?
A bulging disc occurs when the disc extends outside its normal boundary but remains intact. A herniated disc is more severe, as the inner gel-like core has actually broken through the outer wall. Herniated discs are more likely to irritate nearby nerves and cause significant pain, numbness, or weakness.
When should I see a doctor for a herniated disc?
Consider seeing a specialist if your pain is not improving after a few days of rest, if it radiates down your arm or leg, or if you are experiencing numbness, tingling, or muscle weakness. Seek immediate medical attention if you develop loss of bladder or bowel control, as this may indicate a serious condition such as cauda equina syndrome.
Will I need surgery for a herniated disc?
Most herniated disc cases do not require surgery. The majority find relief through conservative treatments such as medications and epidural steroid injections. Surgery is typically considered only when symptoms are severe, disabling, or have not responded to several months of non-surgical treatment. Dr. Woska at Shore Spine & Pain will always explore the least invasive options first.
What can I do at home to manage herniated disc pain?
Staying gently active, avoiding prolonged bed rest, and applying ice or heat to the affected area can help manage discomfort. Over-the-counter anti-inflammatory medications may also provide relief. Avoid heavy lifting and movements that worsen symptoms, and follow the guidance of your pain management specialist before beginning any home treatment routine.